Neurosurgeon vs. Orthopedic Surgeon: How to Choose the Right Spine Specialist
If you’ve been told you need spine surgery, you may already be wondering whether you should see a neurosurgeon or an orthopedic surgeon. The distinction can feel confusing, especially when both specialists may offer similar treatments for the same condition. The honest answer is that the title matters far less than you might think, and Dr. Joel Beckett is in a unique position to explain why.
Dr. Beckett completed dual fellowships in both neurosurgical and orthopedic spine surgery and practices as a neurosurgeon, meaning he has trained extensively in both worlds. What he’ll tell you is that both specialties produce excellent spine surgeons, and each brings something genuinely valuable to the table. Understanding those differences will help you make a more informed decision about your care.
Key Differences Between Neurosurgeons and Orthopedic Surgeons
While neurosurgeons and orthopedic surgeons can perform many of the same spine procedures, their training paths are meaningfully different. Indeed, those differences shape how each type of surgeon approaches the spine. During residency, neurosurgeons train exclusively on the brain, spine and peripheral nerves for seven full years. Orthopedic surgeons spend five years training across the entire musculoskeletal system including knees, hips, hands, and the spine. Orthopedic surgeons need to complete a spine fellowship to specialize in spine care. After completing a seven-year neurosurgery residency, a neurosurgeon is qualified to perform spine surgery immediately; no fellowship is required. Many do complete a fellowship for added subspecialty depth, but the foundational training is comprehensive enough to stand on its own. Importantly, neither path is superior and each produces a distinct set of strengths that complement each other.
Neurosurgeons
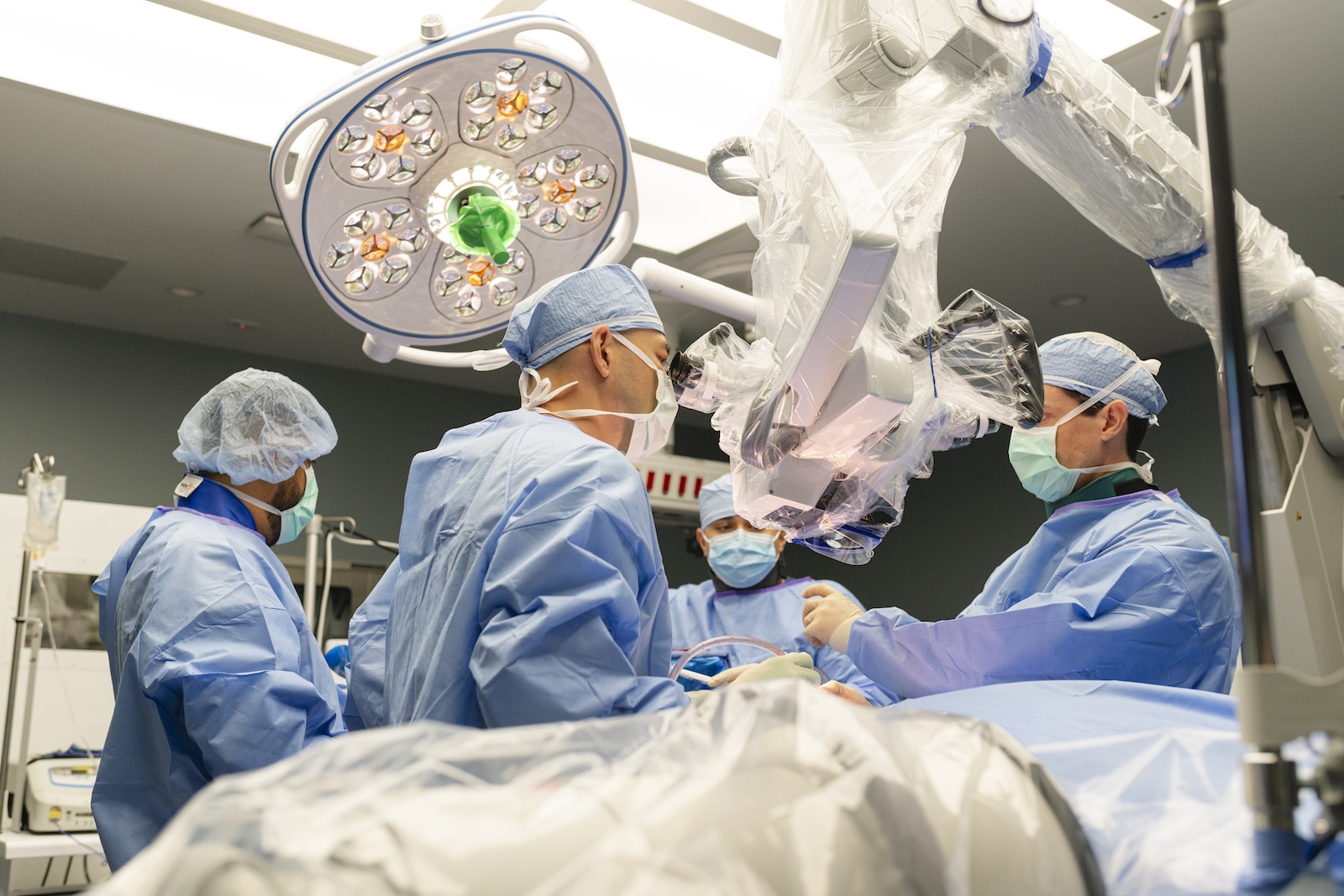
Neurosurgical residency is seven years of surgical training focused entirely on the brain, spine and nerves of our body. From day one, neurosurgery residents are operating with a microscope, developing precision in and around some of the most delicate structures in the human body: the brain, the spinal cord, nerve roots, and the protective membranes that surround them, including the dura.
One of the most serious complications in spine surgery is a dural tear, which is a breach of the membrane that encases the spinal cord and nerves. Managing this complication requires immediate, confident action. Because neurosurgeons spend their entire residency opening and working around nerves and the dural layer, this is familiar territory. Extensive training in intradural surgery, i.e., operations inside the dural sac itself, is exclusive to neurosurgeons. Orthopedic surgeons, regardless of their skill level, cannot perform intradural procedures.
Orthopedic Surgeons
Orthopedic surgeons spend five years residency training focusing on the musculoskeletal system (bones, joints, and ligaments). Trainees operate on knees, shoulders, hips, spine and have experience in most bones and joints in the body. They understand alignment, load distribution, and how structural changes affect function over time.
Unlike neurosurgeons, who are qualified to perform spine surgery immediately after residency, orthopedic surgeons who subspecialize in spine must complete a dedicated fellowship after their five-year training program.
In spine care, this background often translates into a focus on structural correction, instrumentation techniques, and mechanical restoration, particularly when instability, deformity, or multi-level degeneration drives the patient’s symptoms.
Orthopedic spine surgeons commonly manage conditions where spinal alignment has shifted or where the structural integrity of the spine has been compromised. This includes scoliosis, kyphosis, spondylolisthesis with significant slippage, and degenerative changes affecting multiple spinal levels. Their training in fixation, fusion, and reconstruction allows them to address these mechanical problems while also decompressing nerves when compression accompanies the structural issue.
Where They Intersect
Most spine conditions aren’t purely a nerve problem or purely a structural one—they’re both. A herniated disc compresses a nerve because the disc structure has failed. Spinal stenosis narrows the canal because of degenerative bony changes. Treating the spine well almost always requires understanding both sides of that equation.
This is one of the reasons Dr. Beckett pursued dual fellowships in both neurosurgical and orthopedic spine surgery—not because one path was incomplete, but because blending both gave him a fuller picture. He brings the neurologic precision of neurosurgery training alongside the structural and mechanical expertise developed through orthopedic fellowship. The result is a practice built on what he calls a modern, blended approach: treating the whole spine problem, not just the nerve side or the bone side of it.
For patients, the takeaway is straightforward. Rather than asking “neurosurgeon or orthopedic?” ask instead: what is this surgeon’s residency and fellowship training, what is their case volume in my specific condition, and can they manage both the neurologic and structural aspects of my spine? Those questions will tell you far more than any title.
The Most Important Factor: Spine Surgery Training
When choosing a spine surgeon, the most important credential isn’t the title. It’s the depth and focus of their training. For orthopedic spine surgeons, that means a dedicated spine fellowship after residency. For neurosurgeons, who enter spine surgery with seven years of exclusive brain and spine training, it means the quality and focus of their residency experience.
What a spine fellowship is (and why it matters)
A spine fellowship is an additional year of intensive training that occurs after a surgeon completes residency. During this time, the surgeon focuses exclusively on spine surgery, working alongside experienced spine specialists in high-volume centers. This concentrated experience provides exposure to a wide range of spinal pathology, from straightforward decompressions to complex multi-level reconstructions and deformity corrections.
Fellowship training matters because it goes beyond technical skill. Surgeons learn how to manage complications, refine their surgical judgment, and develop the ability to match the right procedure to the right patient. The result is a surgeon who can evaluate your condition with depth, offer a full spectrum of options, and execute the plan with confidence.
What patients should look for related to fellowship training
When evaluating a spine surgeon, start by confirming they completed a spine fellowship. For a neurosurgeon, it’s good to have; for an orthopedic surgeon, it’s essential. This credential signals dedicated, high-volume training beyond residency. If the information is not readily available on their website or practice materials, it’s appropriate to ask directly during your consultation.
Beyond fellowship completion, ask about case volume: “How often do you perform this procedure?” A surgeon who treats your condition regularly will have more refined judgment and technical skill than one who performs the operation occasionally. High case volume also means the surgeon has seen a broader range of outcomes and complications, which translates into better decision-making for your specific situation.
Finally, look for breadth in their surgical toolkit. The best spine surgeons can offer minimally invasive options when appropriate, motion-preserving techniques like artificial disc replacement for suitable candidates, and complex reconstruction when deformity or instability requires it. A surgeon with this range can tailor the operation to your condition rather than defaulting to a one-size-fits-all approach.
Why fellowship + case mix beats the label
Two surgeons can have the same title and vastly different spine expertise. One may perform spine surgery occasionally alongside other procedures, while the other dedicates their entire practice to spinal conditions. The title “spine surgeon” means little without the training and case volume to back it up. A spine surgeon with deep experience in your diagnosis will recognize nuances that others might miss, and they’ll be able to discuss not just what they plan to do, but why other options may be less appropriate in your case.
Dr. Joel Beckett completed two fellowships spanning minimally invasive spine surgery, spinal tumor and complex spinal deformity, giving him expertise across the full spectrum of spinal care. His practice focuses exclusively on spine surgery, with high case volume in procedures ranging from outpatient microdiscectomy to multi-level reconstruction. If you’re evaluating your options for spine surgery, schedule a consultation at Beckett NeuroSpine to discuss your diagnosis, review your imaging, and determine the best path forward for your long-term spine health.
How to Choose a Spine Surgeon: Questions to Ask at Your Consultation
1) “What is my exact diagnosis, and what structure is causing my symptoms?”
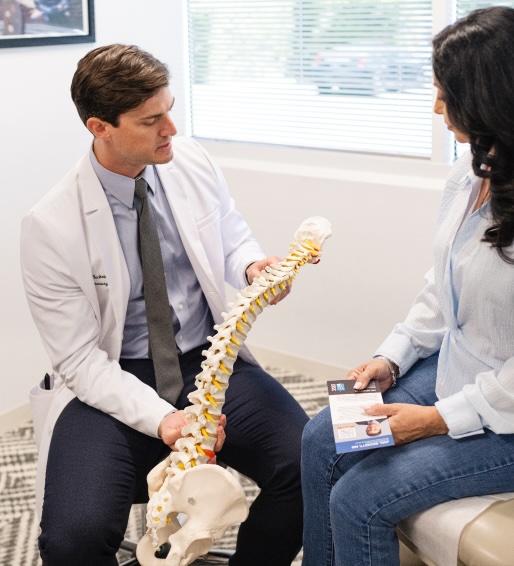
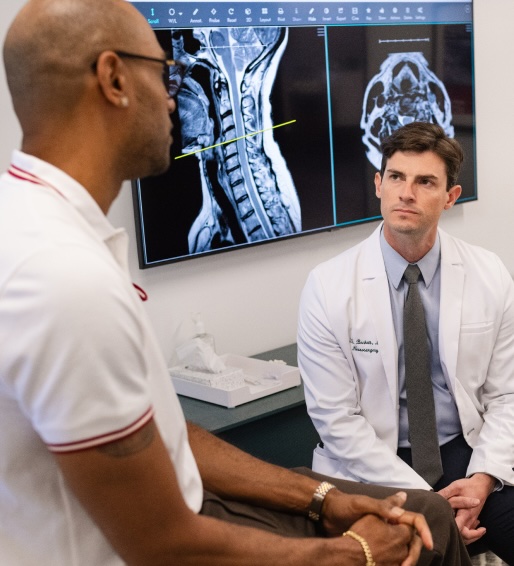
Ask your surgeon to show you on your MRI or CT scan exactly what’s abnormal and what’s driving your pain. A good surgeon will point to the specific disc, nerve, or vertebra involved and explain how that structure relates to your symptoms. This visual review helps you understand whether the problem is a herniated disc compressing a nerve, spinal stenosis narrowing the canal, or instability causing mechanical pain.
Equally important, confirm whether your symptoms match the imaging. Not every abnormality on a scan causes pain, and not every pain comes from an obvious imaging finding. Could it be muscle dysfunction, referred pain, or adjacent segment issues rather than the abnormality on imaging? And when in doubt, get a second opinion.
2) “What are all my treatment options, including non-surgical and less invasive approaches?”
Before agreeing to surgery, ask what non-surgical treatments you can try first, such as physical therapy, targeted injections, activity modification, or anti-inflammatory medication. A good surgeon will outline what signs would indicate it’s time to consider surgery. These include signs and symptoms such as progressive weakness, severe unrelenting pain, or failure of conservative care after a reasonable trial.
If surgery is recommended, ask what less invasive or motion-preserving options may apply to your case. This includes minimally invasive techniques that spare muscle and soft tissue, as well as motion-preserving procedures like artificial disc replacement. A surgeon with a full range of options can tailor the approach to your condition rather than defaulting to a single technique for every patient.
3) “How often do you treat my condition, and how often do you perform this procedure?”
Ask how many cases like yours the surgeon treats and how often they perform the exact procedure being recommended. A surgeon who operates on your condition monthly will have more refined judgment and technical skill than one who performs the procedure once or twice a year. High case volume also means broader experience with variations in anatomy, complications, and outcomes.
Beyond volume, ask what outcomes they track and what complications they see most often. A surgeon who monitors their results and discusses complications openly demonstrates accountability and realistic expectations. This transparency helps you understand not just the potential benefits of surgery, but also the risks and what happens when things don’t go as planned.
4) “[If your case is complex] What’s your experience with complex spine surgery or reconstruction?”
If your surgeon mentions that your case is complex, ask what specifically makes it so. Complexity can come from spinal deformity, multi-level degenerative disease, prior failed surgery requiring revision, or instability that affects alignment and load distribution. Understanding why your case is considered complex helps you evaluate whether the surgeon has the training and experience to manage it safely.
Ask how they plan to protect nerve function while restoring stability and alignment. Complex cases often require balancing multiple goals such as decompressing nerves, correcting alignment, and achieving solid fusion. A surgeon experienced in complex reconstruction will be able to explain their strategy clearly, including how they’ll address both the mechanical and neurologic aspects of your condition.
5) “What does recovery look like for me, and what restrictions should I expect?”
Ask for a realistic timeline for returning to walking, driving, work, and exercise based on your specific procedure and overall health. Recovery varies widely depending on whether you’re having a microdiscectomy, decompression, or fusion, and whether the surgery involves one level or multiple levels. A surgeon who provides tailored expectations rather than generic timelines demonstrates familiarity with how different procedures and patient factors affect healing.
Also ask what symptoms are normal during recovery versus red flags that need urgent follow-up. Understanding the difference between expected post-operative soreness and concerning signs like fever, increasing weakness, or drainage from the incision helps you navigate recovery with confidence and know when to reach out for guidance.
Conclusion: Making the Best Decision for Your Health
In truth, the neurosurgeon vs. orthopedic-surgeon debate misses the point. What matters is finding a spine specialist with dedicated fellowship training, substantial experience treating your specific condition, and the ability to explain your options clearly. Both neurosurgery and orthopedic surgery residencies produce excellent surgeons, but the individual surgeon’s experience, breadth of techniques, and commitment to spine care make the real difference in outcomes.
Dr. Joel Beckett completed dual fellowships in minimally invasive spine surgery and complex spinal deformity, giving him expertise across the full spectrum of spinal conditions. His practice focuses exclusively on spine care, from straightforward decompressions to complex reconstructions, shaped by daily, high-volume clinical experience. If you are evaluating your options or seeking clarity on a recommended treatment plan, schedule a consultation at Beckett NeuroSpine to review your imaging, discuss your diagnosis, and determine the best path forward for your long-term spine health.